Most parents prepare for the birth of their baby with the expectation that they will be bringing their healthy baby home from the hospital within a couple days. Emma has taught us, however, that we should always expect the unexpected. She came into this world in a whirlwind of sickness and complications. Within minutes, we knew of her initial diagnosis of Down syndrome, (a.k.a. Trisomy 21) which the doctor said would have to be confirmed still by a blood test. It was quite apparent, though, from her appearance that this diagnosis was true. She had several physical charecteristics of Down syndrome which the doctor explained to us: creases in the palm of the hands, low-set ears, slightly slanted eyes, and an unusually large gap on both feet between her large toe and the one next to it. Emma was struggling to breath from the beginning, and after working on her for a few minutes, the nurse allowed Lisa to hold Emma. It was a very brief moment, because Emma's breathing quickly got worse and became very labored. Little did Lisa know that she wouldn't get to hold Emma again for almost 2 weeks.
 Emma in the nursery
Emma in the nursery She was taken to the nursery and assessed there by the doctor on call. Jeff went with her while Lisa was left all alone in an empty room wondering what was happening. Things happened very quickly that first hour as she went from being assessed in the nursery to being admitted into the NICU (neonatal intensive care unit). It was very difficult for us as parents to get thrust into a new world of medical terms and acronyms that we didn't understand and it all seemed so scary. A couple hours later, Jeff took Lisa via wheelchair up to the NICU to meet with the neonatologist. He discussed with us their intial assessment of Emma. She had an infection and was still struggling to breathe. He started discussing with us in more detail how many babies with Down syndrome are born with congenital heart defects, which in turn can cause pulmonary hypertension. They felt like this was the most likely cause of her breathing struggles. He went on to talk about the possibility of intubation if her breathing didn't improve. They also scheduled an echocardiogram for the next morning to look for heart defects, which meant a high probablity of open heart surgery... It was a rough night.... The next morning ("Black Thursday" as it became known) they had already intubated Emma during the night and the echocardiogram showed no defects (lucky girl!). The x-ray of her lungs, however was not so promising. She did, in fact, have pulmonary hypertension believed to be complicated by her abnormally shaped lungs. The doctor said her lungs looked like the Liberty Bell, which became her first nickname.

Thursday morning in the NICU
By Thursday afternoon, Emma's condition continued to decline. They explained that her infection had spread throughout her body by entering the bloodstream, also known as newborn sepsis. The regular ventilator wasn't enough to sustain her breathing, so they switched her to a high frequency oscillatory ventilator. Her blood pressure was dangerously low, admist other complications. This was the first time we were faced with the possiblility of losing our newborn baby. Nothing in the world can prepare you to face that reality...

 We looked like crap and felt like it, too. (the smiles were very forced...)
We looked like crap and felt like it, too. (the smiles were very forced...)That night, Emma took another turn for the worse. She was "maxed out," as they called it, on life support. They were giving her the max doses of her life-sustaining medications and her only option was ECMO, a heart/lung support machine. Basically, her body was shutting down and we made the decision to move forward towards ECMO, which meant a transfer to another hospital. The closest hospital with this capability was Primary Children's Medical Center, where she was taken by LifeFlight around 5:00 a.m. Friday morning. Emma arrived at PCMC in critical, but stable, condition (a shock to all of us). A fighter was born in Emma for the first time, as her condition slowly started improving after arriving. She was still very, very sick, but ECMO was put on the back burner. PCMC became our new "home away from home." Over the next couple days, Emma swelled up like a balloon and gained 3 pounds because they were constantly giving her IV fluids to sustain a stable blood pressure.

 Her second nickname became "Sumo Baby," it was so sad!
Her second nickname became "Sumo Baby," it was so sad!The next 3 weeks consisted of ups, downs, and more ups and downs. It was a rollercoaster ride of strained emotions combined with gradual improvements in Emma's condition. We were dealt a crash course in NICU technology and terminology. We spent our first holiday in a hospital (Thanksgiving), and Lisa finally got to hold her baby (vent tubes and all) after 12 long days.
 Lisa was in heaven!
Lisa was in heaven!Emma continued to get better and we did eventually get to bring her home. As long as this post has been, it doesn't do this experience justice. It was a bitter-sweet experience through it all.
 Emma's coming home day. Notice the outfit barely fits that we had bought prior to her birth as a "coming home" outfit. This was about the only time she wore it...
Emma's coming home day. Notice the outfit barely fits that we had bought prior to her birth as a "coming home" outfit. This was about the only time she wore it...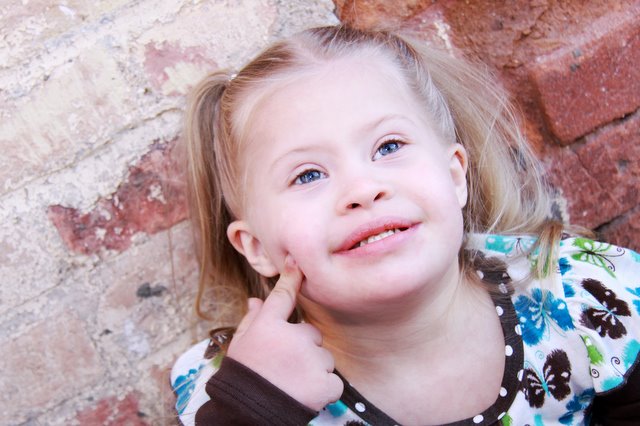











No comments:
Post a Comment